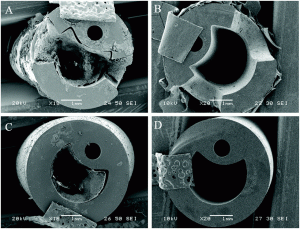
Intraluminal Catheter Encrustation. Photo Credit: Royal Society of Chemistry. http://pubs.rsc.org/-/content/articlehtml/2017/tb/c7tb01302g.
Pearl: There is likely little advantage gained from treating asymptomatic bacteriuria in patients with chronic indwelling foley cathethers. If you will not treat it, you probably should refrain from testing it.
Question: Some like to play fast-and-loose with the bacteria found in chronic indwelling foleys. If you need a source upon which to blame patient behavior/symptoms, it will always be there for you. If you want to send the patient home, you can claim the colonization is chronic and meaningless. What if you do the latter, but the patient comes back a few days later with a UTI? Should you have just thrown some antibiotics at it “to be safe?”
Answer: Probably not. To start with, there is a nice review published in CID in 2009 (1) from which I am now claiming expertise. They review cases in their hospital of patients who had foley catheters and received IV antibiotics to treat a UTI and classified them (ex-post-facto) into appropriate treatment of CAUTI versus inappropriate treatment of CAABU (catheter-associated asymptomatic bacteriuria). They note that the CDC confusingly still functionally classifies the latter as a sub-type of UTI, leading many hospitals to fear non-payment by CMS for these findings. However, they cite a number of studies, including this (2) which suggest that colonization of all foley cathethers begins within the first 24 hours and is nearly 100%, and often poly-microbial, in patients with chronic cathethers. Moreover, they furnish this (3) article in which the authors performed routine cultures on chronic foley patients and gave half cephalexin every time a sensitive organism grew out regardless of symptoms while the other half only received treatment when symptoms or vitals signs were supportive. There were no differences in clinical outcomes but the always-treat group developed a lot more cephalexin resistance.
Bottom-line: Patients with chronic foley catheters are almost universally colonized. I did not find data supporting treatment of positive cultures in the absence of new symptoms or signs of active infection. Moreover, obtaining cultures when not indicated is likely to result in a CAUTI for the hospital if they are inpatient. Lastly, if you ARE obtaining cultures, there is some data that you will obtain better cultures if you place a new catheter before taking your sample.
Dedication: Thank you to Dr. Andrus and Dr. Taub for providing the impetus for this clinical pearl.
Sources:
(1) Inappropriate treatment of catheter-associated asymptomatic bacteriuria in a tertiary care hospital. Cope M, Cevallos ME, Cadle RM, Darouiche RO, Musher DM, Trautner BW. Clin Infect Dis. 2009 May 1;48(9):1182-8. PMID: 19292664
(2) A prospective microbiologic study of bacteriuria in patients with chronic indwelling urethral catheters. Warren JW, Tenney JH, Hoopes JM, Muncie HL, Anthony WC. J Infect Dis. 1982. Dec;146(6):719-23.
(3) Cephalexin for susceptible bacteriuria in afebrile, long-term catheterized patients. Warren JW, Anthony WC, Hoopes JM, Muncie HL Jr. JAMA. 1982 Jul 23;248(4):454-8.