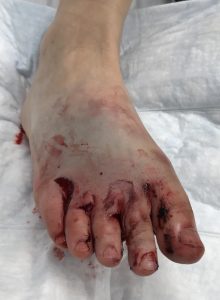
In a totally hypothetical situation, imagine a resident’s foot got run over by a bus and looked like this after arriving in your ED…
What sort of things should you be concerned about in injuries like this of extremities?
1. Vascular: Has a vessel been compromised, especially an artery? It is important to control hemorrhage. Are pulses palpable or dopplerable? Are they symmetric? Is there a bruit or enlarging hematoma? If there is any doubt without signs of active ischemia, consider vascular imaging like a CTA. Otherwise, immediately call vascular and/or IR and/or surgery depending on who is available in your hospital, and orthopedics. Venous bleeding can still be life-threatening. Depending on the location, certain fractures are more likely to cause injury to certain vasculature.
2. Nerve: Check both sensation and motor, being aware of what nerves are more likely to be injured.
3. Bone: Bony injuries including fractures and dislocations should be high on your differential given the forceful sudden impact. a) Look immediately for deformities that would suggest a joint dislocation that may require an expedited reduction, like the ankle, in order to preserve blood flow. b) Get that XR and maybe a CT or MRI depending on your suspicions. c) Consider that there are definitely some open wounds in this case. If there is an underlying fracture, they may need to be treated as open fractures, so give antibiotics and make sure their tetanus is up to date. Involve orthopedics early. Depending on the injury, they may a cast vs cam boot vs OR. Remember Lisfranc injuries can be easily missed – injury to the tarsometatarsal joint complex, where many times you see displacement between the second metatarsal and middle cuneiform and thus displacement of the third through fifth metatarsals.



4. Muscle: There is bound to be swelling. If there is a vascular injury or as the swelling expands, it is important to think about compartment syndrome. Yes, you can get compartment syndrome of the foot. Is the extremity starting to look like it is dying (pain, pallor, poikilothermia, paresthesias, pulseless, paralysis)? It can lead to muscular compromise and can be limb threatening. Depending on the extent of swelling, it wouldn’t be unreasonable to observe for a period of time to do neurovascular checks. Crush injuries like this can lead to rhabdomyolysis and all that comes with that. It is important for patients to stay hydrated.
5. Soft tissue: a) Clean the wound thoroughly to rid it of debris. b) Sutures may be necessary. If there are just lacerations and they are around joints with concern for joint space involvement, you may consider injecting the joint with saline to see if there is then outflux from the laceration wound, i.e. a saline load test (SLT, how much you inject depends on the joint, often times methylene blue is added). Degloving injuries can happen because of the rotational/shearing nature, causing traumatic separation of skin and subcutaneous fat from deeper soft tissue. These free-floating parts can more easily become ischemic and slough off. These sorts of injuries definitely require antibiotics. Depend on the severity, some may require going to the OR for debridement and stabilization.
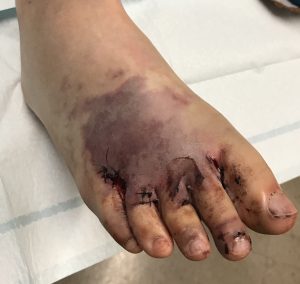
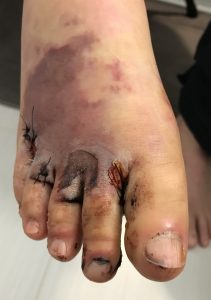
Here’s what the hypothetical foot may look like 3 and 6 days after…
Give patients warning signs of infection, ischemia, and DVT. Follow up care is important to set up and may include further imaging like an MRI. Rest, ice, compression, elevation.
Beware of buses! Hide your wife, hide your kids.
Resources:
https://www.uptodate.com/contents/severe-extremity-injury-in-the-adult-patient?search=degloving&source=search_result&selectedTitle=2~12&usage_type=default&display_rank=2
https://www.uptodate.com/contents/tarsometatarsal-lisfranc-joint-complex-injuries?topicRef=114170&source=see_link