A 1-week-old infant is brought in by his mother for decreased responsiveness and vomiting. Prenatal and birth history were unremarkable. He is cool, clammy, and lethargic. Nurses are unable to obtain a blood pressure, and he is hypoglycemic to the 30s. You establish IV access, send labs, and administer fluids and dextrose. He then begins to have a seizure.
Your differential should be broad include a congenital cardiac disease, sepsis / infectious process such as meningitis, an intracranial process, metabolic derangement, GI or nutritional disorder, abuse, etc. The lab helps guide your differential as they call to report some critical values: sodium 120 and potassium 6.5.
TL;DR – When you see hypotension, hypoglycemia, hyponatremia, and hyperkalemia – think adrenal crisis, fix metabolic derangements, and administer stress dose steroids.
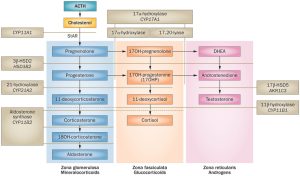
Congenital adrenal hyperplasia (CAH) is a group of inherited disorders that results in impaired steroid synthesis. Remember these pathways?
Enzymes impaired at any step of the hormone production pathways result in a unique combo of elevated precursors and deficient products. The most common form of CAH is 21-hydroxylase deficiency.
Severe cases of 21-hydroxylase deficiency may precipitate an adrenal crisis. Insufficient aldosterone secretion leads to poor sodium reabsorption in the kidneys, resulting in salt wasting. Patients also have a cortisol deficiency and excess of androgens (easy to understand if you follow the pathyway).
ED Treatment:
Stress dose steroids: Hydrocortisone 1-2 mg/kg IV bolus (though can give 25 mg to neonates)
And don’t forget to correct underlying metabolic and electrolyte derangements.
Hyponatremia causing CNS dysfunction: Treat with Hypertonic Saline 3% 3cc/kg over 10-30 minutes
Pearl inspiration courtesy of Dr. Michelle Vazquez’s awesome low-fi sim case this morning.
References:
https://www.ncbi.nlm.nih.gov/books/NBK279085/
http://emedicine.medscape.com/article/919218-overview
http://www.nature.com/nrendo/journal/v10/n2/fig_tab/nrendo.2013.239_F2.html
http://www.chop.edu/clinical-pathway/steroid-stress-dosing-and-weaning-clinical-pathway
http://www.medscape.com/viewarticle/557966_8
http://reference.medscape.com/drug/a-hydrocort-solu-cortef-hydrocortisone-342744