Thanks to Tatiana for an expertly presented ultrasound case of the month. She was kind enough to put together this summary.
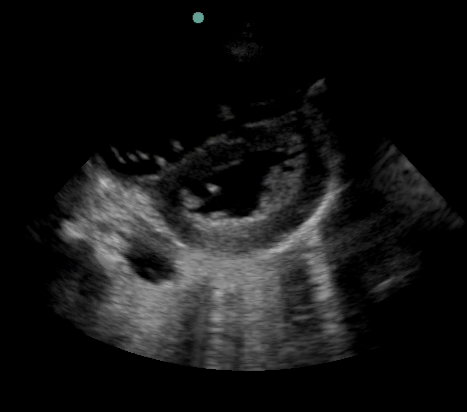
43y.o. F with pmh of asthma, HTN, recently treated for PNA p/w worsening dyspnea, pleuritic chest pain, cough and fever. Found to be tachypnic and tachycardic in the ED. CXR suggesting perihilar PNA. While awaiting chest CTA to r/o PE you perform bedside echo and obtain the following image:
Is there anything abnormal? How does this change your management?
This is a parasternal short axis view showing dilatation of RV, D-shaped LV and flattening of ventricular septum, consistent with RV strain.
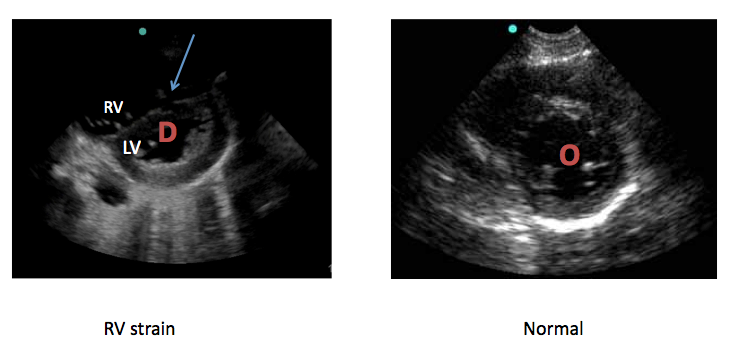
Below are side-by-side parasternal views of heart with RV strain and normal heart. Arrow points to flattened ventricular septum.
Why one should perform an echo when suspecting PE?
- Prognosis – stable patients with PE and RV strain have increased mortality and increased rate of recurrent PE
- Therapy – consider more aggressive treatment (i.e. thrombolytics) in patients with RV dysfunction
- Response to therapy
- Rule out other causes (i.e. pericardial effusion and tamponade)
Signs of PE on echo:
Thrombus in right heart or right sided vasculature, dilatation of RV, RV hypokinesis, flattening of ventricular septum, dilatation of pulmonary arteries, dilated IVC, significant TR, decreased LV cavity size.
Back to the case. The patient had multiple subsegemental and segmental pulmonary emboli on CT angio and was started on heparin therapy. She was admitted to ICU and was intubated on day 2. Patient did not receive thrombolytics and still remains in the ICU.