The following scenario is based on a case that was seen in the Sinai ED this past week.
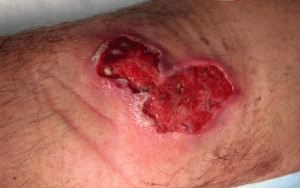
A 52 yo M with hx of poorly controlled DM and HTN p/w rapidly progressing ulcer over the past 3 weeks of right lower extremity. He has been afebrile and has normal vital signs in the ED. Of note he just returned from Cameroon after living there for 5 years. The ulcer has the following appearance:
What could it be you ask? In this case it was a Buruli ulcer.
A Buruli ulcer is caused by Mycobacterium ulcerans. It is is a chronic disease that affects skin and bone. Transmission of the disease is not currently known but it is believed to be associated with contaminated water sources in wetland areas. It is most commonly found in West Africa but may also be seen in Mexico, South America, China, Japan, and Australia.
In terms of severity, the disease has been classified into three categories: Category I – single small lesion (32%), Category II – non-ulcerative and ulcerative plaque (35%) and Category III – disseminated and mixed forms such as osteitis, osteomyelitis, joint involvement (33%). The disease often starts as a painless nodule or a large painless area of induration. Because of local immunosuppressive properties the disease often progresses in the absence of pain or fever. Without treatment, the nodule or area of induration erodes within 4 weeks creating the classical appearance of an ulcer with undermined borders. Occasionally, bone can be affected as well which causes visible deformities of the affected area.
there are currently four laboratory tests which can be used to confirm the diagnosis: IS2404 polymerase chain reaction (PCR), direct microscopy, histopathology and culture. PCR is the most commonly used method. The World Health Organization offers a guide on all of these testing modalities.
There are two different treatment options for Buruli ulcers. Both regimens require 8 full weeks of antibiotic treatment. They are as follows:
- a combination of rifampicin (10 mg/kg once daily) and streptomycin (15 mg/kg once daily)
- a combination of rifampicin (10 mg/kg once daily) and clarithromycin (7.5 mg/kg twice daily). This regimen is preferred in pregnancy.
Additional treatment with urgical debridement and wound care is also necessary for many of these patients. Physiotherapy and long term rehab may also be required depending on the extent of involvement of the ulcer.