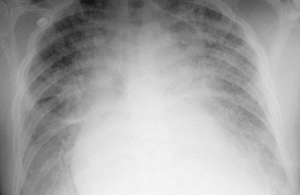
Many ER residents have found themselves justifying an admission of an acute or decompensated heart failure patient to a skeptical admitting resident. For better or worse, the skepticism is not without reason; an initial ED admission diagnosis of AHF (acute heart failure) in ED is discordant from final discharge diagnosis in about one out of four cases. But finding that one test to definitively diagnose AHF remains allusive. A recent meta-analysis in Academic Emergency Medicine found fairly unimpressive LR’s of the most common testing modalities for AHF. Take a look at these numbers:
Signs of fluid overload on CXR: +LR 4.8-6.5
B-lines on bedside lung ultrasound: +LR 7.4 and -LR 0.16.
S3 on auscultation: +LR 4.0
BNPs <100: -LR 0.1
BNPs >500:+LR 4-9
So while a negative BNP is helpful in excluding AHF, and a lung soon is (mildly) helpful in making the diagnosis, the likelihood ratio of any of these tests individually is not great.
Read more:
Martindale J, et al. “Diagnosing Acute Heart Failure in the Emergency Department: A Systematic Review and Meta-analysis” Academic Emergency Medicine. 2016;23:223–24