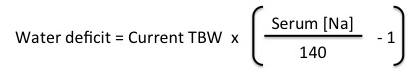Clinical Scenario: A 66-year-old male with a past medical history of traumatic brain injury and frequent urinary tract infections sent from his nursing home with hypernatremia. On a routine blood draw he was found to have hypernatremia to 160. His mental status is unchanged. How do you correct his hypernatremia?
Hypernatremia is caused by
- Excessive water loss: gastrointestinal tract (vomiting or diarrhea), sweating, or urination, renal, third spacing (loss of hypotonic fluid)
- Signs: dry mucous membranes, decreased skin turgor, orthostatic changes
- Hypertonic sodium gain (iatrogenic)
- Often causes acute hypernatremia
Steps to correct
STEP 1: Calculate water deficit
- TBW = lean body weight x %
- Young: 60% male or 50% female
- Elderly: 50% male or 45% female
- Calculate water deficit
STEP 2: Choose rate of correction
-
- Acute hypernatremia (<48 hours)
- Goal to lower acutely to 145mmol/L within 24 hours
- Chronic hypernatremia (>48 hours)
- Goal lower maximum 10mEq/L in 24 hours (0.5mEq/L/hour)
- The rate should not exceed this to avoid cerebral edema
- Re-check sodium every 2 hours
- Acute hypernatremia (<48 hours)
Step 3: Calculate Fluid Repletion
- Acute (< 48 hours)
- Hourly infusion rate (mL/hour) > water deficit in mL/24 hours
- Chronic (> 48 hours)
1. Pick infusate based on volume status. More hypotonic solutions require less volume.
- Free water via oral or peg tube if mentating well
- D5, 1/4 NS, or 1/2 NS if unable to take by mouth
- Only use normal saline if the patient is hypotensive, orthostatic, or with frank hemodynamic compromise.
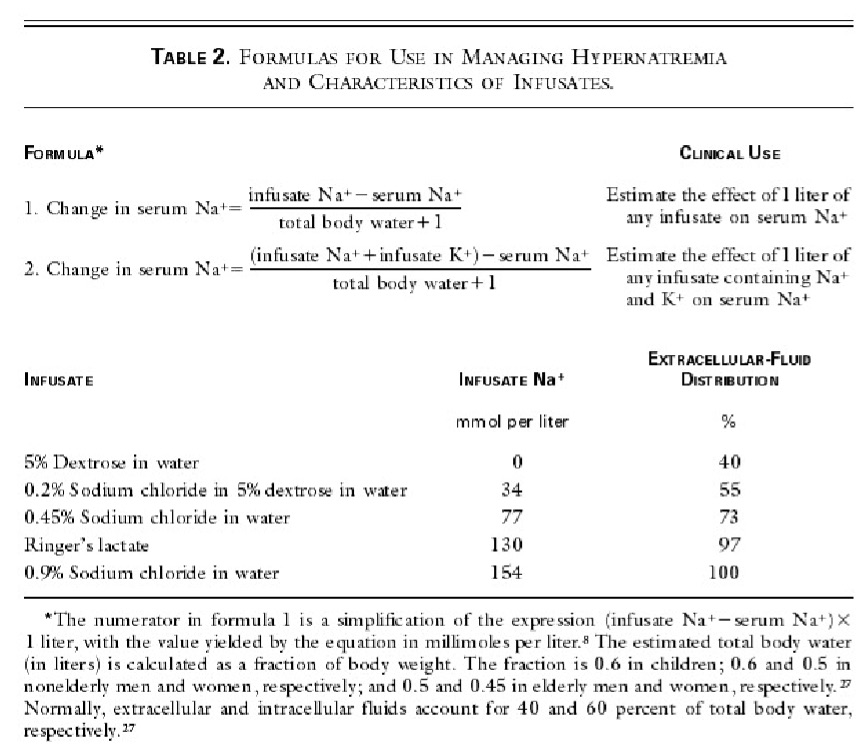
2. Calculate change in serum sodium

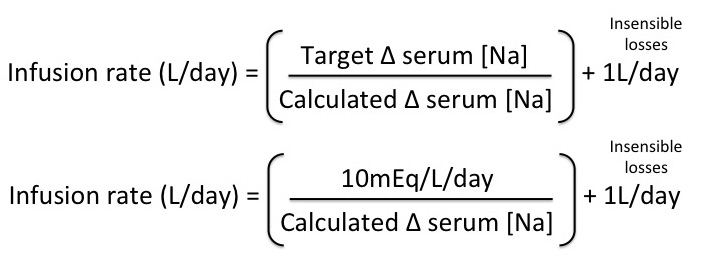
3. Calculate the infusion rate
- Infusion rate (L/d) = Target change in serum Na / Calculated change in serum Na = 10mEq/L / Calculated change in serum Na
- Account for insensible losses by adding 1 L/day and you get the infusion volume/day
Back to the case… this was CHRONIC hypernatremia
Step 1:
- TBW = lean body weight x 50% = 70kg x 50% = 35kg
- Water deficit = TBW x (Serum [Na]/140 – 1) = 35 x (160/140 – 1) = 5 L
Step 2:
- Goal: 0.5mEq/L/hour or 10mEq/L/day
Step 3: In this case we will use 0.45% NaCl as the patient is moderately hypovolemic
- Change in serum Na = (infusate Na – serum Na)/(TBW +1) = (77-160)/35 + 1) = -2.3 mmol
- 1/2NS infusion rate = 10mEq/L / 2.3 mEq = (4.34 L + 1L)/24 hours = 220 mL/hour
Or… alternatively you can use MDCalc …Free Water Deficit or Sodium Correction
References/Additional resources (Accessed 12/30/16)
- Adrogue HJ, Madias NE. Hypernatremia. N Engl J Med. 2000;342(20):1493-1499.
- If you prefer podcast form http://emcrit.org/podcasts/hypernatremia/
- Free water deficit calculator http://www.mdcalc.com/free-water-deficit-hypernatremia/
- Sodium correction in hyper/hyponatremia http://www.mdcalc.com/sodium-correction-rate-hyponatremia-hypernatremia/