Last week, we closed out the week by discussing the dischargable, ‘benign sugars,’ but what about when you have the legit ‘sugars.’ We’re talking about DKA. While the algorithm for DKA is fairly straight forward – fluids, insulin, replete lytes prn, admit / ICU consult, there are some often under appreciated subtleties we neglect in the ED. Let’s start with fluid choice.
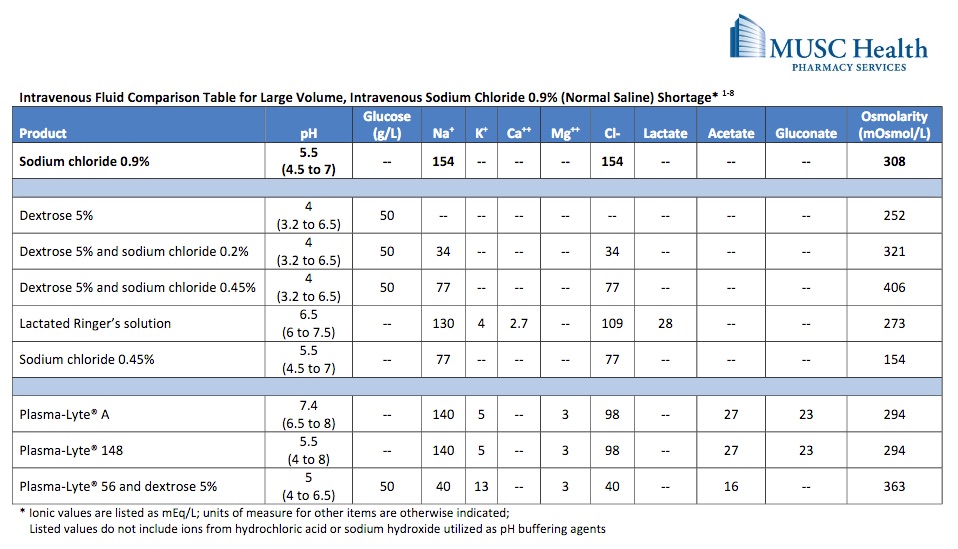
Most clinicians empirically start volume resuscitation with 0.9% saline or ‘normal saline.’ As we’ve all heard, there is very little truly normal about normal saline. Specifically in the context of DKA, one should worry about giving an acidic solution (with a pH of ~5.5) to an already acidotic patient. Other, perhaps more savvy clinicians reach for isolyte / plasmalyte. With a more physiologic pH, logically this makes sense, however one must be weary of giving potassium to a patient population that is typically hyperkalemic (often due to normal fluid shifts of acid base balance). So let’s review some of the most commonly used ED fluids:
This is clearly a complicated question, so what do the ‘experts’ do. Uptodate recommends resuscitation with 0.9% saline at a rate of 15-20 mL/kg/hour. The American Diabetes Association similarly recommends initial resuscitation with 0.9% NS. So what should you do…? There is no clear right answer, so check a gas and choose wisely.
References:
Kitabchi AB, Hirsch IB, Emmett M. Diabetic ketoacidosis and hyperosmolar hyperglycemia state in adults: treatment. Uptodate. Nathan DM, Mulder JE (EDs). http://www.uptodate.com/contents/diabetic-ketoacidosis-and-hyperosmolar-hyperglycemic-state-in-adults-treatment?source=search_result&search=dka+fluid&selectedTitle=1%7E150
Kitabchi AE, Umpierrez GE, Miles JM, Fisher JN. Hyperglycemic Crises in Adult Patients With Diabetes. Diabetes Care 2009 Jul; 32(7): 1335-1343. http://dx.doi.org/10.2337/dc09-9032
MUSC Health Pharmacy Services. Intravenous Fluid Comparison Table for large volume, Intravenous Sodium Chloride 0.9% (Normal Saline) Shortage: http://academicdepartments.musc.edu/medicine/divisions/pulmonary/fellowship_and_education/education/Critical%20Care%20Syllabus/critical_care_files/Resuscitation/saline%20iv%20fluid%20comparison.pdf Jan 2014
Umpierrez G. Korytkowski M. Diabetic emergencies – ketoacidosis, hyperglycaemic hyperosmolar state and hypoglcaemia. Nature Review Endocrinology. 12. 222-232 (2016. Doi:10.1038/nrendo.2016.15
