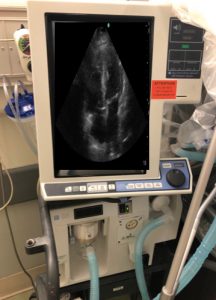
This pearl will be a brief rundown of the hemodynamic effects of BIPAP on the patient with sympathetic crashing pulmonary edema. This is an apical four chamber view with a dilated right ventricle – stretched vertically to the point of being almost unrecognizable – superimposed on the screen of a ventilator.
Yes.
BIPAP works for sympathetic crashing acute pulmonary edema (SCAPE) – we know this – how it works was not obvious to me for a long time. Fluid doesn’t just get pushed out of the lungs.
Positive pressure ventilation (PPV) increases the intrathoracic pressure while the systemic vasculature remains at atmospheric pressure. The increase in pressure around the heart creates an unfavorable pressure gradient for blood to return to the heart. Preload is decreased with positive pressure ventilation. Dropping preload is a problem for many patients (see: critical aortic stenosis). However, patients with SCAPE have failing ventricles that need to do less work, and need less preload. Moreover, gasping for air creates huge negative intrathoracic pressures, and pulls in even more preload (more work, more failure).
So, preload drops with PPV, but what about afterload?
The increase in intrathoracic pressure created by PPV increases the LV transmural pressure. The increased LV transmural pressure relative to the transmural pressure of the systemic vasculature (stuck at atmospheric pressure) creates a more favorable pressure gradient for blood to follow out of the thorax. Afterload is decreased with positive pressure ventilation. Patients with SCAPE have a catecholamine surge which drives up their systemic vascular resistance, and increases afterload. PPV decreases afterload, and in doing so unloads work from a failing ventricle.
The deranged physiology blog offers offers an outstanding explanation with diagrams.
References:
“Effects of Positive Pressure Ventilation on Cardiovascular Physiology.” Deranged Physiology, 27 Aug. 2016, www.derangedphysiology.com/main/core-topics-intensive-care/mechanical-ventilation-0/Chapter%202.1.7/effects-positive-pressure-ventilation-cardiovascular-physiology.
Tobin, Martin J. Principles and Practice of Mechanical Ventilation. McGraw-Hill Medical, 2013.