Title: “The 52 in 52 Review: PE Rule Out with Wells and D-dimer”
Article Citation: Wells PS, Anderson DR, Rodger M, Stiell I, et al. Excluding pulmonary embolism at the bedside without diagnostic imaging: Management of patients with suspected pulmonary embolism presenting to the emergency department by using a simple clinical model and D-dimer. Annals Intern Med 2001;135:98-107. PMID: 11453709
What we already know about the topic: Pulmonary embolism has a high mortality if untreated. Determining pretest probability and using high negative predictive value of d-dimer may simplify diagnostic process.
Why this study is important: Clinical signs and symptoms of pulmonary embolism are not specific and diagnostic testing may be time-consuming or may not be available. Previously, the use of D-dimer to exclude pulmonary embolism has been limited in the ED. In addition, the diagnostic algorithm (Wells Criteria) to classify pretest probability of pulmonary embolism has not been tested in the ED. In this study, the authors assessed the safety of combining Wells Criteria with d-dimer to manage patients suspected of pulmonary embolism in the ED.
Brief overview of the study:
The study design was a prospective cohort study in 4 Canadian hospitals. Patients were evaluated by 1 of 43 ED physicians who used Wells Criteria to determine a pre-test probability of pulmonary embolism. For each patient, a D-dimer test was also performed.
Inclusion: suspicion of PE, symptoms for <30 days, acute onset of new or worsening shortness of breath or chest pain
Exclusion: suspected DVT, no symptoms of PE within 3 days of presentation, AC > 24 hours, expected survival time <3 months, contraindication to contrast media.
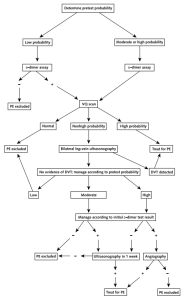
There were 930 patients in the study. Each patient was evaluated with the same diagnostic algorithm (see figure). For patients with a low pretest probability and a negative D-dimer, no further tests were done and were given the diagnosis of PE excluded. For all other combinations of pretest probability and d-dimer, patients undergone VQ scans and the diagnosis of PE excluded was given further down the algorithm. After 3 months, patients were followed up for development of thromboembolic events.
5/849 patients had the diagnosis of PE excluded at one point of the algorithm developed PE or DVT during follow-up. However, 4 of these patients had not undergone the proper diagnostic protocol.
1/ 437 patients who had the initial diagnosis of PE excluded developed PE during follow up. The negative predictive value for combining low Wells score and negative D-dimer is 99.5% (CI, 99.1% to 100%)
Limitations:
Clinical gestalt is heavily weighted using Wells criteria. Each item of Wells criteria is not mutually exclusive.
CTA has replaced VQ scan, because CTA has better sensitivity and specificity. Maybe the miss rate of thromboembolic events would be higher if CTA was used.
Take home points:
Pulmonary embolism has a high mortality if untreated. Managing PE patients using pretest probability and d-dimer may simplify diagnostic process and decrease the need for diagnostic imaging.