We’ve all seen that movie where some old person coughs into a handkerchief and as the camera slowly pans away, there’s some blood stain. You know that guy isn’t making it to the end of the movie…

Today, let’s talk about a less commonly featured troupe: Massive Hemoptysis
Massive Hemoptysis is defined as hemoptysis > 1000ml in a 24 hour period, a fact that is not nearly as useful as the patient’s acute presentation but a question that comes up sometimes.
Cause: 95% of massive hemoptysis arise from bronchial circulation; a series of arteries fed directly from the aorta and with a mean arterial pressure 5 times higher than what is supplied in the pulmonary arterial circulation. Now onto the good stuff
Management: The important part of management is ABCs!
Airway:
The important thing for these patients is identifying whether or not they are protecting their airway.
How frequently do they expectorate blood, what volume of blood coming up, their spO2, their work of breathing, etc.
If the decision is made to intubate, a large-bore ET Tube should be used, preferably 8.0 or larger. This will be helpful for removing clots as well as for bronchoscopy afterward by Pulmonology. I would recommend either:
- Intubation with a bougie
- A smaller tube and then exchange-over-bougie to place a large-bore ET tube
- ETT-over-bronch if there is time for DSI.
Breathing:
Due to the blood filling the alveoli and blocking the bronchioles, these patients are prone to V/Q mismatch and shunt physiology; therefore, become hypoxic relatively easily.
- If not intubated, HFNC would probably be preferable. You don’t want to put a mask over a person who’s actively coughing up blood.
- If intubated, lay the person with the affected lung facing downward. This will help prevent bleeding into the non-affected lung to improve
- One could also advance the ETT and mainstem the non-affected lung in order to ventilate only the non-affected lung. This is much easier if the affected lung is the left one.
Keep in mind for one lung ventilation, the tidal volumes should be halved and the respiratory rate should be adjusted to maintain normal minute ventilation.
Pulmonology should be consulted early for bronchoscopy. Both for stopping the bleeding and to help with the removal of these bad boys
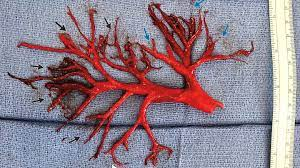
Circulation:
- Blood transfusions as needed.
- Reverse known causes of coagulopathy
- Again, early consultation of Pulmonology to assist with hemorrhage control. They have many different options available to staunch bleeding that are beyond the scope of this pearl.
- If the patient is stable or has a definitive airway, then a CTA would be beneficial to help identify cause and/or source of bleeding. In some cases, IR may be involved as well for an embolization.
